RCM that scales with your clinic
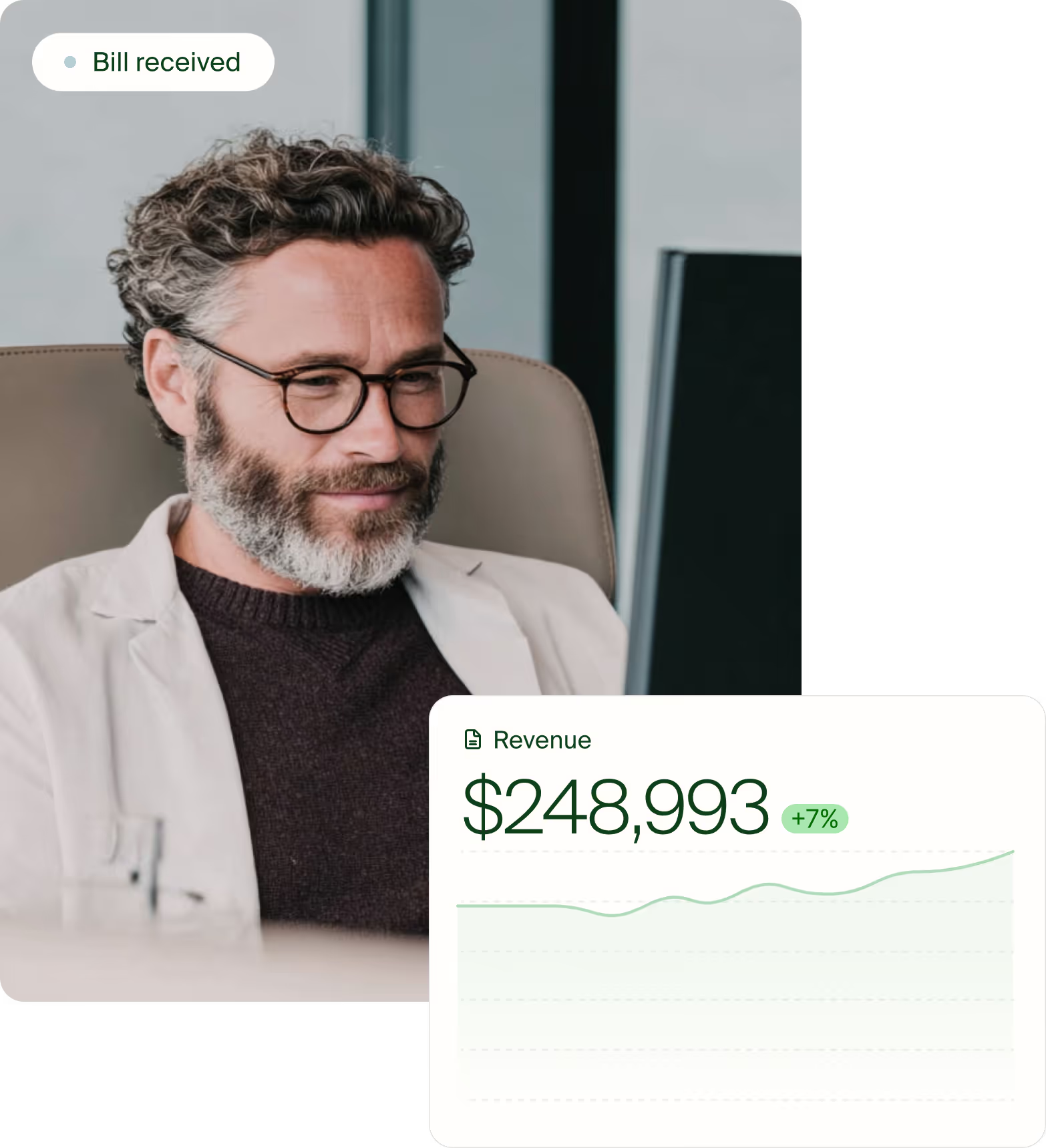
Our onshore billing team is supported by proprietary AI trained on millions of behavioral health claims.
Everything you need from an RCM team
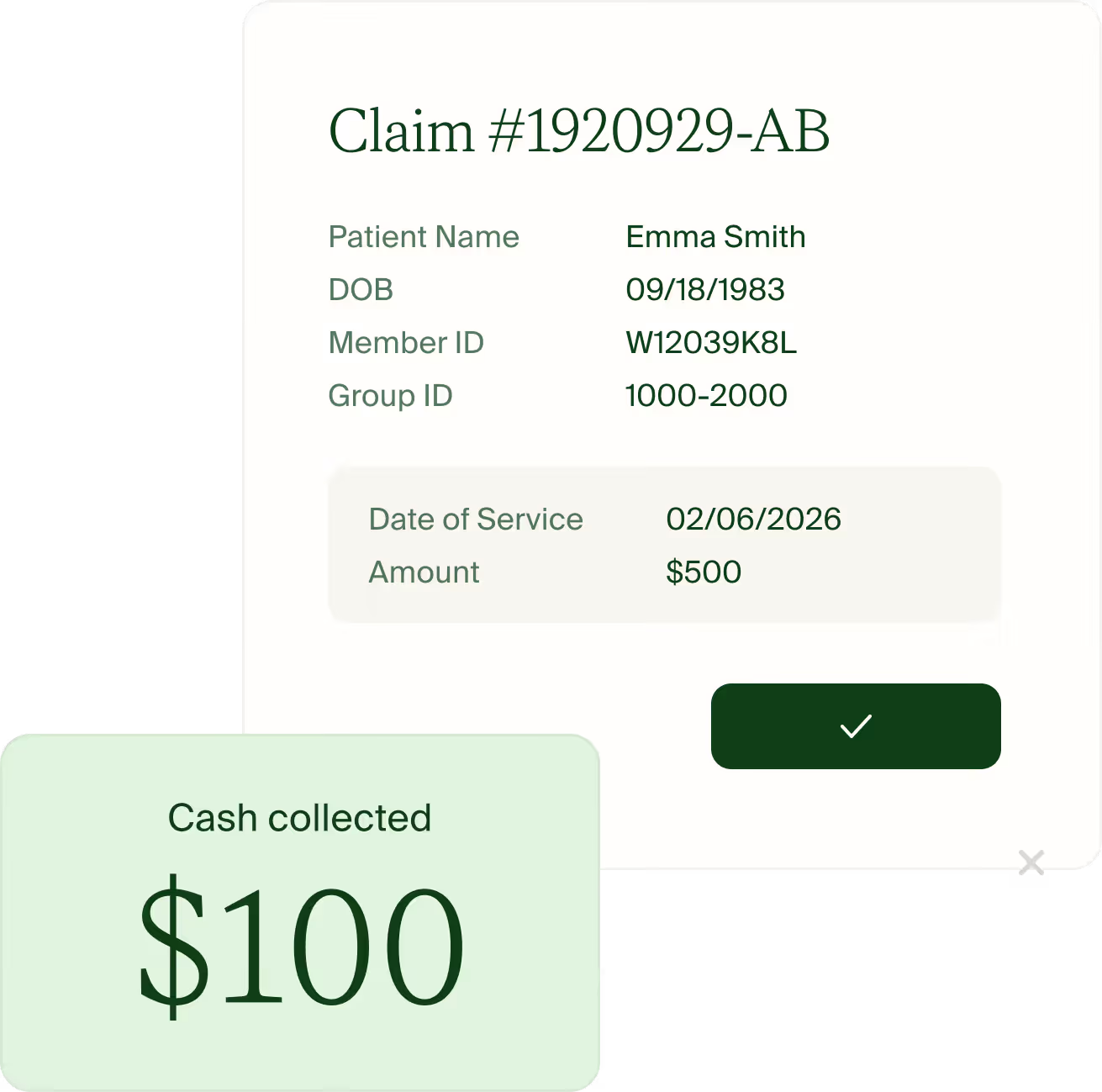
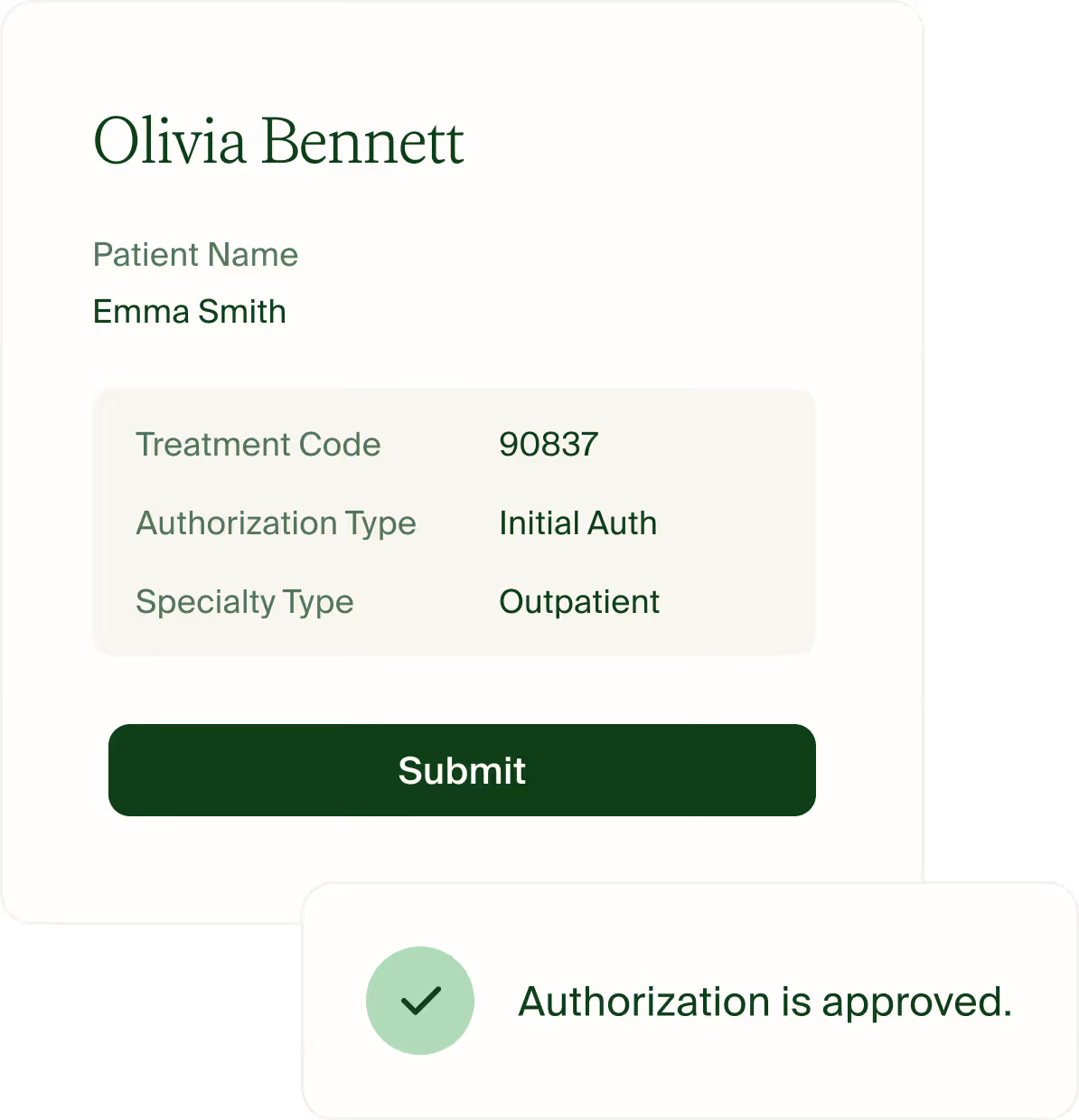
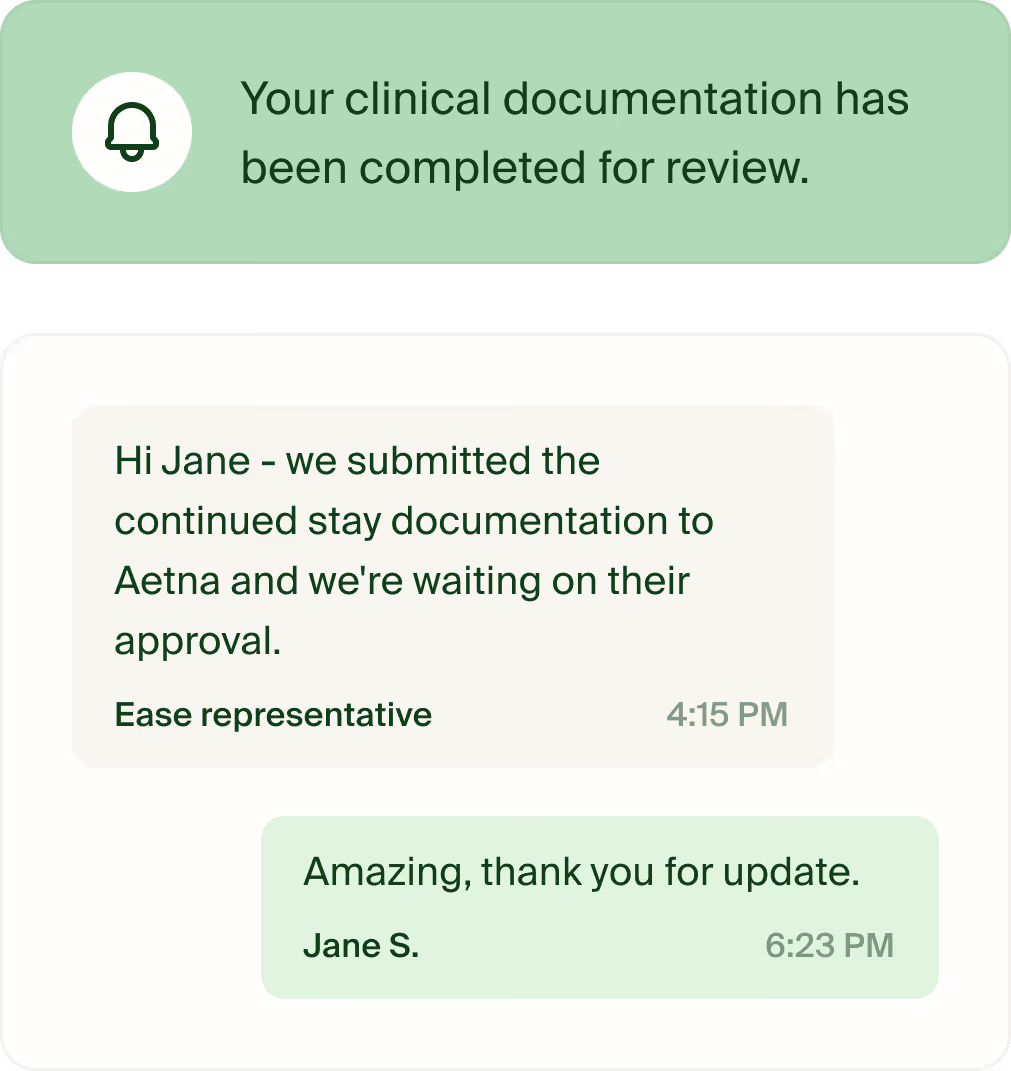
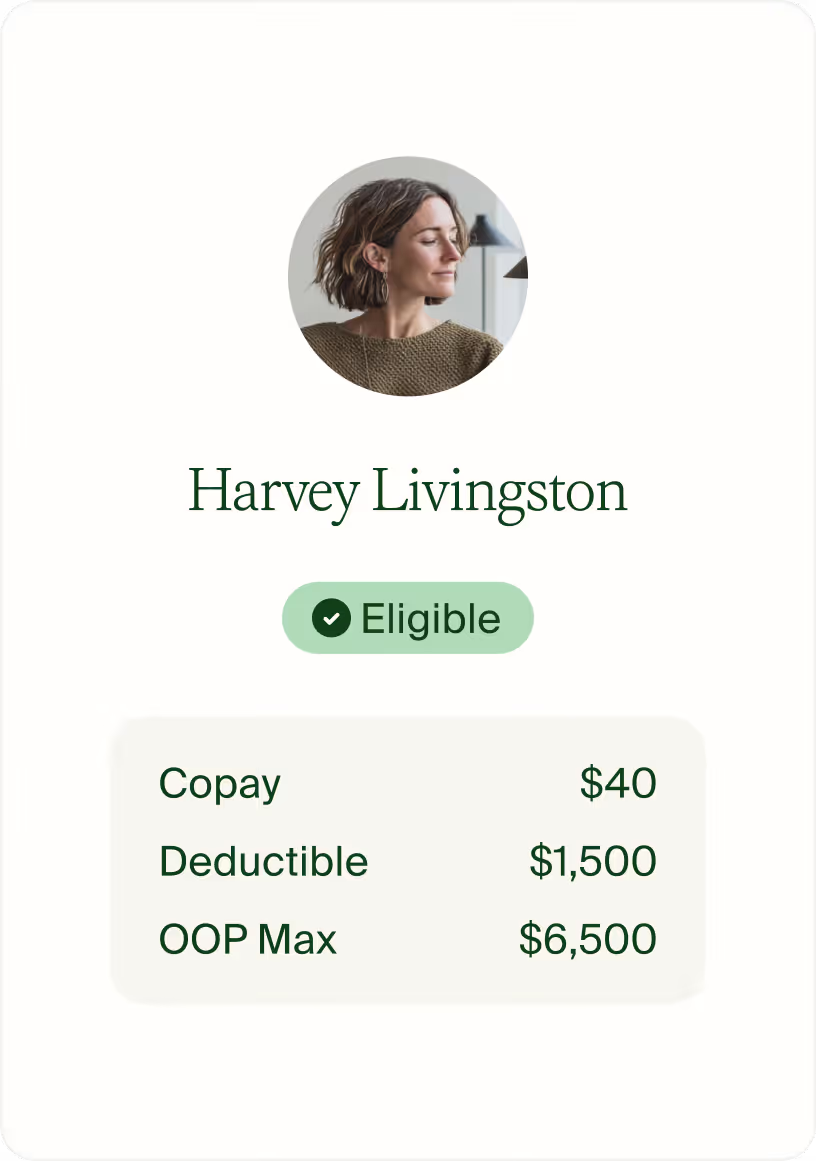
What it’s like working with Ease
Have an in-house billing team? Our RCM engine is best in class.
Claims
Worklist
rules engine
Parsing
FAQ
AI-trained billing intelligence automates validation, flags denial risks, prioritizes follow-ups, and accelerates cash flow.
We support organizations nationwide across diverse state-specific billing and regulatory requirements.
Metrics include acceptance rates, denial rates, days in A/R, reimbursement timelines, payer performance, and clean claim rates.
Live Power BI dashboards provide visibility into claims, collections, aging, denials, and payer performance.
Yes. Electronic remittances are set up and managed for all clients.
We support most behavioral health EHR and practice management systems.
End-to-end RCM services include authorization, credentialing, eligibility, billing, denials, payment posting, and manual claims.
Flexible pricing is offered per-claim or as a percentage of collections with tiered volume-based rates.
